
Fax: (860) 430-9693
Glastonbury, CT 06033

Chondromalacia patella, also known as Patellofemoral Syndrome is a specific type of knee arthritis that affects the cartilage on the back of the kneecap (the patella). The name "chondromalacia" comes from chondro, referring to cartilage, and malacia, meaning softening or irritation. However, it's important to note that you can have Patellofemoral Pain Syndrome (PPS) without having the cartilage damage seen in Chondromalacia Patella. We offer solutions for treating patellafemoral pain syndrome in Glastonbury, CT at Valley Sports Physicians & Orthopedic Medicine.

Patients typically complain of pain around or behind the kneecap. Symptoms are worsened by physical activity, especially running and jumping. Prolonged sitting causes pain when attempting to stand back up. Also, going downstairs or inclines can cause pain, more so than going up. Some patients report grinding, catching or locking behind the kneecap. Swelling can also occur. Young athletes are more affected than adults, and girls seem to be more affected than boys.
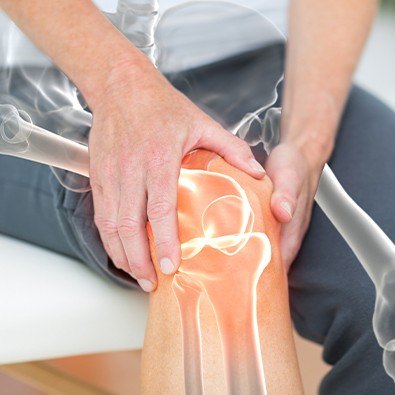
Learn More About the Q-Angle of the Knee
Ideally, treating CM/PPS should target the underlying cause(s). Biomechanical problems, such as flat feet, should be addressed. For flat feet, the vast majority of patients do not need to spend the excessive amount of money (in our opinion!) that most podiatrists and therapists charge for custom orthotics. Off-the-shelf orthotics, such as Superfeet®, work well in most cases. (For convenience you can buy Superfeet orthotics in our office!)
Dysfunction of the gluteus medius muscle needs to be addressed when present. The problem is that the vast majority of physical therapists don't know how to train the gluteus medius properly to perform its stabilizing function. They instruct patients in high load strengthening exercises. But this isn't the main problem. The real problem is that the gluteus medius doesn't fire in the proper timing sequence, it's not a strength-weakness issue. Delayed contraction of the muscle allows the knee to rotate inward. So therapy needs to work on retraining muscle firing patterns, not strengthening the muscle.
Patellar stabilizing braces and straps to help control patellar tracking can be useful to keep the symptoms under control, but they do nothing to fix the underlying problems. Special patellar taping techniques, such as McConnell Taping, to help control patellar tracking can also be helpful to control symptoms.
When conservative measures such as physical therapy, orthotics, and bracing/taping don't help, more aggressive treatment may be needed. We've had very good success using Regenerative Medicine treatments, such as Prolotherapy/Prolozone, PRP, and stem cell injections.* These treatments are intended to stimulate the body's natural healing and repair mechanisms to heal the damaged cartilage and to tighten the ligaments that stabilize the patella. We've been performing these treatments longer than most physicians in the country. Click the box below to get our free Regenerative Medicine e-book. It's important to keep in mind that biomechanical problems and muscle imbalances still need to be fixed - Regenerative Medicine treatments complement these treatments; they don't replace them. Surgery is always a last resort for treating Chondromalacia.
(*NOTE: All Regenerative Medicine treatments are performed by our affiliate practice, the New England Stem Cell Institute. Click HERE for a free e-book on Regenerative Medicine.)